Get your IUD inserted at Everywoman’s
An IUD (intrauterine device) is a very effective, convenient, long acting birth control method and have high satisfaction rates compared to other methods. IUDs don’t require remembering anything (like taking a pill every day) and are safe for people who cannot use birth control containing estrogen.
They can be removed at any time by a doctor if you do not like it or want to get pregnant. IUDs are rapidly reversible, meaning that fertility returns very quickly after removal.
If you are getting a hormonal IUD you should not have unprotected sex for at least seven days before your appointment, and for seven days afterward. After that a hormonal IUD is extremely effective at preventing pregnancy.
A copper IUD is effective immediately and is the most effective form of emergency birth control if it is inserted within seven days of unprotected sex.
What kinds of IUDs are there?
This page has more information on the different types of IUDs.
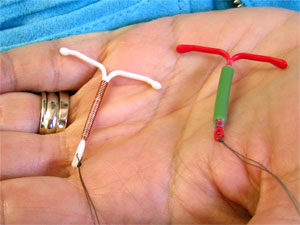
Copper IUD on the left, hormonal IUD on the right.
Why come to us for an IUD?
~ Our doctors are highly skilled and have put in thousands of IUDs. Research shows that IUD insertions are safer and more comfortable with experienced doctors.
~ We can help you decide what IUD is best for you, based on the most up-to-date medical research.
~ We use local anesthetic to reduce discomfort with IUD insertions.
~ We do on-site ultrasounds before and after each insertion to ensure that the IUD is correctly placed.
~ We are usually able to help even if you have challenging or complicated IUD insertion issues.
~ We do sexually transmitted infection testing at same time as IUD insertions and offer Pap testing if you are due for one.
~ We are able to insert IUDs at any time during your cycle (you do not need to be on your period at the time of insertion).
Costs and coverage
IUDs can be inserted at the time of an aspiration abortion for after the followup appointment with a medical abortion and are free for anyone with MSP. Costs are approximate as pharmacies may have slightly different fees: copper IUD $80, Mirena or Kyleena $400. The cost for those without MSP may be covered in whole or in part by extended medical insurance. The clinic fee for those without insurance is $325.
Your IUD insertion
The doctor puts some freezing into your cervix, measures the size of your uterus and inserts the IUD. You may have a pinching feeling and a sharp cramping pain for a few minutes.
You may or may not feel some dizziness, sweating and/or nausea after the insertion. You may have some bleeding as well; please bring a pad with you. You will be asked to rest for at least 10 minutes after the insertion to ensure that you are okay to leave.
If you have an IUD inserted at the time of an aspiration (surgical) abortion, it is done during the procedure and there is usually very little discomfort. If you make an appointment just to have an IUD inserted, it helps to take some Ibuprofen (Advil) before your appointment.
After the insertion
You can expect to have some cramping and spotting (on and off bleeding or brown discharge) in the first few months, especially in the first two weeks and sometimes lasting as long as six months. Take ibuprofen or acetaminophen for the cramps.
With a hormonal IUD: your period will usually get much lighter than normal after the first few months, and sometimes stop completely (this is completely safe).
With a copper IUD: you can expect your regular period to come at its usual time. Your period is likely to be heavier and longer, especially in the first three to four months. We recommend you take ibuprofen (Advil) or naproxen (Aleve) all the way through your period for these first months to reduce cramping and bleeding. You may also have some cramping and/or on and off bleeding, spotting or brown discharge outside of your period in the first few months – this is normal.
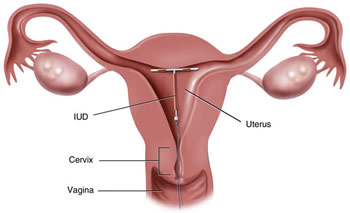
Checking your IUD
IUDs have soft strings that hang through the cervix. These are used by a health care provider to remove the IUD. After your period (or every month), you can check to see if you are able to feel the strings of the IUD by putting your finger inside to the top of your vagina. If you can’t feel the string, the string feels shorter or longer than the last time you checked, or if you feel any hard plastic, then get your IUD checked by a health care provider.
You may want to check the strings more often during the first six weeks. This is because there is a small chance of the IUD coming out (expulsion). If this happens, it is most likely to happen in the first six weeks.
If your hormonal IUD is expelled and we find out before six weeks have passed, the drug company may replace it. So, if your Mirena or Kyleena comes out in the first six weeks and you notice it happening, keep the IUD and call us right away.
It is also recommended to have the IUD checked by a health care provider every year or at any time you are feeling that something has changed.
What to watch for
In addition to the very small chance of pregnancy or expulsion (the IUD coming out), there is about a very small chance of perforation (the IUD going into the wall of the uterus), which will usually heal after about two weeks with no long term side effects. This may sometimes require laparoscopic removal of the IUD (a small procedure). There is also an extremely small increased risk of infection in the first three weeks following insertion. If you have fever or chills, a smelly discharge from your vagina, or unusual lower abdominal (belly) pain that does not feel like cramps, see a doctor or call the clinic to make a follow up appointment. If you become pregnant with an IUD, risks are rare, but you should see a doctor as soon as possible.
Please note: some health care providers have out of date information about IUDs – if someone advises you to remove your IUD or warns you of risks or side effects not included here, please contact us.
If you have questions or concerns about the IUD, you can fill out our contact form or call us at 604-322-6692. You can also contact Sex Sense through www.sexsense.org. or 1-800-739-7367.

